Introduction
That “simple ankle sprain” might be hiding a critical diagnosis—a dorsal navicular avulsion fracture. For chiropractors, imaging centers, and attorneys, missing this is the difference between 6 weeks of healing and 6 months or more of chronic, sometimes debilitating pain. With the right diagnostic pathway, professional imaging consultants and board-certified DACBRs (Diplomates of the American Chiropractic Board of Radiology) can spot this injury, issue a targeted radiology report, and guide successful treatment from the start.

Case Presentation: When “Ankle Pain” Isn’t Just an Ankle Sprain
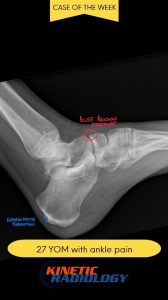
A 27-year-old male recreational soccer player presented to the clinic with persistent dorsal foot and ankle pain following an inversion-type injury incurred during a weekend game. Initially diagnosed as a mild ankle sprain, he experienced persistent discomfort and localized tenderness along the dorsal midfoot, especially with dorsiflexion and push-off activities. Swelling was modest but focal, with no gross deformity or instability.
Follow-up radiographs revealed a small, sharply marginated fragment arising from the dorsal aspect of the navicular bone—clearly visible on the lateral view. Subsequent review by a DACBR (Diplomate of the American Chiropractic Board of Radiology) confirmed the findings, issuing a targeted radiology report that explicitly diagnosed a dorsal navicular avulsion fracture.
This diagnosis explained the patient’s ongoing pain and guided appropriate management, shifting the treatment plan from typical ankle sprain rehabilitation to immobilization and restricted weight-bearing. The case underscores the essential role of professional imaging consultants and diagnostic imaging specialists in identifying subtle midfoot injuries that are commonly overlooked.
Bilateral Cervical Ribs, with anatomical features correlating to clinical symptoms of left-sided neurogenic *Thoracic Outlet Syndrome (TOS)*.
The navicular bone is integral to midfoot stability, articulating with the talus and cuneiforms, forming the keystone of the medial longitudinal arch. The dorsal surface is a crucial anchor point for the dorsal talonavicular ligament and the tibionavicular fibers of the medial deltoid ligament.
Key Point for DACBRs and Imaging Consultants: The dorsal portion has a relative watershed in blood supply, heightening risk for poor healing if avulsed.
Avulsion Mechanism: Hyper-dorsiflexion or inversion generates tensile stress, often via ligamentous pull, resulting in a cortical “flake” avulsion of the dorsal navicular.
Typical Clinical Setting
Initial clinical diagnosis is frequently “ankle sprain,” but subtle bony pain on the dorsal midfoot—especially in the context of these mechanisms—should raise suspicion for this injury, especially among diagnostic imaging consultants and radiologists.
Standard X-ray Evaluation
Expert DACBRs emphasize the challenge: small dorsal navicular avulsion fractures can be tough to spot on ankle and foot radiographs. Careful scrutiny of AP, oblique, and especially lateral projections is needed.
Findings:
Professional Imaging Consultants’ Tip:
Always compare with the contralateral foot for accessory ossicles or variant anatomy. Insist on high-resolution lateral views in uncertain cases. Direct reporting language in the radiology report helps drive clinical escalation when the injury is confirmed.
Sample Radiology Report Phrase:
“Small dorsal cortical fragment at the navicular bone, consistent with avulsion fracture. Recommend correlation with clinical findings and possible advanced imaging assessment by a Diagnostic Imaging Consultant or DACBR.”
CT: Detailing the Bone
Computed tomography has become the gold standard for detailed evaluation:
MRI: The Soft Tissue Perspective
MRI, favored by many advanced imaging specialists and DACBRs, is invaluable for:
When to Escalate:
If standard radiographs are inconclusive but clinical suspicion remains, a low threshold for MRI/CT referral is strongly recommended in best practice guidelines for diagnostic imaging consultants.
Misdiagnosis remains a risk without advanced imaging and expert interpretation. Here is an SEO-optimized, comparison-style table for professional imaging consultants, teleradiologists, or those preparing a radiology report:
Diagnosis | Typical Location | Morphology (Imaging) | MRI Findings | Clinical Context | Report Guidance |
Dorsal Navicular Avulsion Fracture (Target DX) | Dorsal navicular | Sharp, cortical fragment | Marrow edema | Acute trauma, ankle sprain | Explicit as “Acute avulsion fracture”; refer for orthopedic/foot specialist |
Os Naviculare (Accessory) | Medial navicular margin | Well-corticated, rounded/oval | No edema | Variable; often asymptomatic | State as “Incidental os naviculare—no acute findings.” |
Navicular Stress Fracture | Central or dorsal navicular | Linear, sometimes sclerotic | Marrow edema, more diffuse | Overuse, repetitive load | “Stress reaction/fracture—athletic injury pattern.” |
Dorsal Osteophyte | Dorsal navicular/cuneiform | Irregular, broad-base | Absent | Chronic, OA changes | “Degenerative bony spurring (osteophyte)—chronic, not acute.” |
Tarsal Coalition | Adjacent to navicular | Osseous, cartilaginous bar | Variable | Rigid or painful foot in youth | “Possible tarsal coalition; further imaging (CT) suggested.” |
DACBR Note:
Differentiating the dorsal avulsion fracture from a small os naviculare, especially in young athletes, is a common challenge encountered on imaging studies performed by professional imaging consultants and diagnostic imaging experts.
A DACBR provides a crucial service beyond simply spotting the anomaly. The radiologist’s report will characterize the cervical rib’s morphology (e.g., complete vs. incomplete, presence of a pseudoarthrosis), which has clinical implications. By identifying this key anatomical variant, the DACBR provides the treating clinician with a definitive underlying cause for the patient’s complex symptoms. This diagnostic clarity allows the provider to move beyond non-specific neck and arm pain diagnoses and implement a highly targeted treatment plan addressing the specific biomechanics of the thoracic outlet.
Every day, chiropractors face the same frustration: imaging reports that miss what matters. General radiologists weren’t trained in your world; they don’t understand subluxations, joint dysfunction, or the biomechanical findings that drive your treatment decisions.
The result? Delayed care. Uncertain patients. Cases that stall when they should be progressing.
The Kinetic Radiology Difference: Chiropractors Reading for Chiropractors
Our board-certified DACBRs aren’t just radiologists. We’re chiropractors who chose to specialize in musculoskeletal imaging. We speak your language because we’ve stood where you stand.
Reports You Can Act On Immediately – No vague findings. No irrelevant details. Just the specific insights that guide your next adjustment, your treatment plan, and your patient conversations.
Same-Day Turnaround – Your patients don’t want to wait days wondering what’s wrong. Neither should you. Get clarity fast so care never stalls.
Documentation That Protects Your Practice – Whether it’s insurance requirements, legal protection, or patient records, our reports give you the clinical backing you need.
Confidence That Builds Your Reputation – When patients see you consulting with specialized radiologists, they recognize your commitment to excellence. That trust turns into loyalty, referrals, and five-star reviews.
Think about the last complex case you handled. Did the radiology report actually help you—or did you have to fill in the gaps yourself?
Now imagine having a DACBR partner who catches the subtle findings, flags the red flags, and gives you confidence in every diagnosis.
No commitment. No risk. Just submit your next challenging case and experience what specialized chiropractic radiology can do for your clinical confidence and patient outcomes.
Questions? Call us at 321 325 0096 or email at support@kineticradiology.com
It is a small fracture where a ligament pulls a chip of bone off the top (dorsal aspect) of the navicular bone in the foot.
This injury occurs when the strong talonavicular ligament creates extreme tension on the bone, causing a fragment to tear away. While it may look like a small “chip” on an X-ray, it is a legitimate fracture that requires proper care. A generic read might miss this, but a DACBR (Diplomate of the American Chiropractic Board of Radiology) is trained to identify these subtle cortical disruptions to ensure the radiology report accurately reflects the severity of the injury.
It usually happens during an ankle sprain, specifically when the foot twists inward while the toes are pointed down.
The mechanism of injury is almost identical to a lateral ankle sprain—plantar flexion combined with inversion. Because the mechanism is the same, clinical exams often focus on the ankle ligaments rather than the midfoot. When Diagnostic Imaging Consultants review these cases, we look specifically at the dorsal navicular area on the lateral view to ensure the source of pain isn’t overlooked.
The symptoms mimic an ankle sprain, and the bone fragment is often small and easily missed by non-specialists.
Pain from this fracture is often masked by the swelling of the surrounding soft tissue. On a standard quick-read, the small bone fragment can be mistaken for noise or a normal variant. However, a detailed radiology report from a specialist will note the jagged edges and lack of cortication, distinguishing a fresh fracture from a chronic sprain.
An avulsion fracture is a fresh break with jagged edges; an Os Supranaviculare is a smooth, normal extra bone you were born with.
This is the most common diagnostic pitfall. An Os Supranaviculare is a congenital accessory ossicle with smooth, rounded, corticated borders. A fracture will have irregular, non-corticated margins. It takes the trained eye of a DACBR to differentiate these subtleties, preventing a patient from being treated for a broken bone when they actually have normal anatomy.
A DACBR is a board-certified chiropractic radiologist with the highest level of training in musculoskeletal imaging.
General radiologists often focus on life-threatening pathology or gross fractures. A DACBR, however, specializes in biomechanics and subtle musculoskeletal injuries common in chiropractic and orthopedic populations. When Diagnostic Imaging Consultants handle your imaging, you get a radiology report that considers the chiropractic context—improving diagnosis and case management.
Partnering with a DACBR teleradiology service provides more than just a second opinion; it offers a significant return on investment:
Speed: Get expert reports in hours, not days.
Expertise: Access board-certified specialists without having to hire them.
Convenience: The entire process is handled online from your office.
Clarity: Receive clear, concise reports that are clinically relevant to chiropractic care, not generic medical reports.
Posted onTrustindex verifies that the original source of the review is Google. Kinetic radiology has been an absolute game changer in speed of reports and detailed reports. Any other doctors I send my reports to are amazed at the detail and the pathology that gets picked up. This is my one and only radiologist group, im thrilled.Posted onTrustindex verifies that the original source of the review is Google. Rishi provides an outstanding service—fast, reliable, and incredibly reassuring. He’s quick to respond, efficient in his work, and always takes the time to address any concerns with clarity and professionalism. I highly recommend his services to anyone looking for a dependable DACBR.Posted onTrustindex verifies that the original source of the review is Google. Prompt efficient service that is thorough and clear. Spinal information is top notch and I've had patients discover kidney stones and possible issues with a hip joint replacement loosening as incidental findings that supported both me and the patient above expectations.Posted onTrustindex verifies that the original source of the review is Google. Quick, accurate, and easy to work with. My new radiology team!Posted onTrustindex verifies that the original source of the review is Google. Excellent, timely reads. Invaluable for CBCTPosted onTrustindex verifies that the original source of the review is Google. Best turnaround time and thorough reports out of any radiologist I’ve seen or worked with!Posted onTrustindex verifies that the original source of the review is Google. Very detailed reports and quick service. Highly recommendedPosted onTrustindex verifies that the original source of the review is Google. Fast turn around time for the radiology reports! Thank you for making this process as seamless as possible!Posted onTrustindex verifies that the original source of the review is Google. I am a NUCCA chiropractor located in Wauankee Wisconsin and I can tell you Dr. Rishi is the only radiologist I’d work with. Sure there are many others in my area but when you want the best you go to the best. He is very easy to work with and always fast to respond and report. 100% recommend.Posted onTrustindex verifies that the original source of the review is Google. Kinetic Radiology is great! They were able to read and get a report written immediately. They are my go to company for any and all images that I need read!Load more
We service all 50 U.S. States, including the following States and Cities listed below.
Copyright 2024 Kinetic Radiology All Rights Reserved
Website Privacy | Terms of UseReceive timely resources to keep you and your practice on the cutting edge of Chiropractic Radiology.
Copyright 2024 Kinetic Radiology
All Rights Reserved
Receive timely resources to keep you and your practice on the cutting edge of Chiropractic Radiology.